In November 2021, doctors at Midwest Gastrointestinal Associates in Omaha got what might be considered a new assistant.
Called GI Genius, the new computer-aided system was designed to help doctors performing colonoscopies identify — in real time — suspicious tissue that might be a polyp, or precancerous lesion in the colon.
The Medtronic device puts a little green box on any spot it thinks might be a polyp, using the same display screen a doctor is watching while navigating the colon’s twists and turns and searching for suspicious spots.
Finding and removing the lesions is important because it decreases a patient’s risk of developing colon cancer, said Dr. Jason Cisler, a gastroenterologist and the practice’s quality chairman. Studies have shown that doctors find more polyps if they have two people looking at the screen.
People are also reading…
After adopting the system, the group’s already good adenoma detection rate — the rate at which doctors find and remove polyps during screening colonoscopies — went up 10% across the board, putting the practice at more than double the national standard. Every 1% increase in the detection rate, according to one study, decreases patients’ risk of colon cancer by 3%.
“It makes it a more sensitive screening tool,” Cisler said. “And what we’re doing is screening. If we’re able to prevent more colon cancer, that’s the rationale where we’re at today.”
The device, approved by the Food and Drug Administration in early 2021, uses a type of artificial intelligence. And it’s just one of a number of technologies incorporating various forms of artificial intelligence that are already working behind the scenes in Nebraska hospitals and clinics. And with research and development underway around the world, there will be more.
Some are focused on flagging doctors about needed health screenings and identifying hospitalized patients at higher risk of being readmitted to the hospital or developing potentially life-threatening infections. Others monitor patients at risk of falling and analyze the impact of blockages in heart arteries on blood flow.
AI also is being used to take some mundane tasks off the plates of both clerical staff and health care providers, freeing them to do higher-level work.
Some Nebraska Medicine doctors are using a product called Dragon Ambient eXperience, or DAX, from a company called Nuance, to capture conversations between themselves and patients and create notes in patients’ charts, said Scott Raymond, the health system’s chief information and innovation officer. The physician then reviews and accepts the notes. Some physicians’ notes now are proving accurate with no need for further human intervention between 80% and 90% of the time.
“It’s a great use of the technology,” he said. “It’s taking away physician burnout, the burden of documentation ... where (they) feel they’re practicing medicine and not being documentation specialists.”
Lincoln’s Bryan Health plans to go live with the system in early May. “We think that will (be) a tremendous win for both our patients and our physicians,” said Bridgett Ojeda, that system’s chief information officer.
Raymond said Microsoft plans to put the artificial intelligence chatbot ChatGPT behind the next version of the program. ChatGPT, developed by OpenAI, has been making headlines around the world in recent months. Users would have to decide whether to adopt it.
Such technologies are making it a fun time to be in health care information technology, Ojeda said. Technologists have spent the last two decades getting information out of paper files and into electronic systems. Now AI and large language models like ChatGPT are allowing them to begin using that data to benefit patients.
Indeed, the authors of a 2022 report from the National Academy of Medicine on AI in health care said their hope is that AI will be the “payback” for investments in electronic systems.
They caution, however, that such systems could introduce bias if not carefully trained and create concerns about privacy and security.
Raymond acknowledged that standards and guardrails need to be put around the technology, particularly when it comes to the chatbots.
Ojeda noted that other challenges lie in having enough health care data and engineering experts to put the technology to work in ways that help rather than disrupt. With interest and investment in the sector high, they have to focus on selecting tools that will be sustainable and ultimately benefit patients.
But Dr. Steven Leitch, vice president of clinical informatics with CHI Health, stressed that humans, not machines, still are making the decisions.
“What would make it scary is if we don’t make the human in charge,” he said. “And that’s not what health care is about. Doctors and nurses make decisions in health care. It’s between people. These tools are amendments; they’re only going to be assisting where we allow them to assist.”
Raymond, who previously practiced as a pediatric intensive care nurse, said Nebraska Medicine and the University of Nebraska Medical Center are forming a committee to consider how the health system will use chatbot technology in research, education and clinical care.
“It’s happening in medicine,” he said. “It’s happening slowly and carefully with a lot of thought behind it. I think it will change how we deliver care and it will improve care. Our responsibility is to make sure we use the technology in the right way.”
The term artificial intelligence, however, implies that machines are reasoning the way humans do, he said. They’re not, although they’re good at gathering data, learning from it and starting to glean insights.
In actuality, Leitch said, what most people think of as “artificial intelligence” really is a broader category that includes a lot of different tools, including machine learning, robotic process automation and the chatbots’ natural language processing. Even chatbots, however, aren’t having independent thoughts but rather are “running very complex sets of rules.”
Cisler said the GI Genius system, also in place at Methodist Endoscopy Center, which is owned by Midwest and Methodist, has been trained on millions of images from colonoscopies and is constantly updated.
But the final word on whether what the system flags actually is a polyp — rather than a bubble or fold in the colon — lies with the doctor, he said.
Such systems, however, also can help sort patients in other ways, and in doing so, make it more likely they get the care they need.
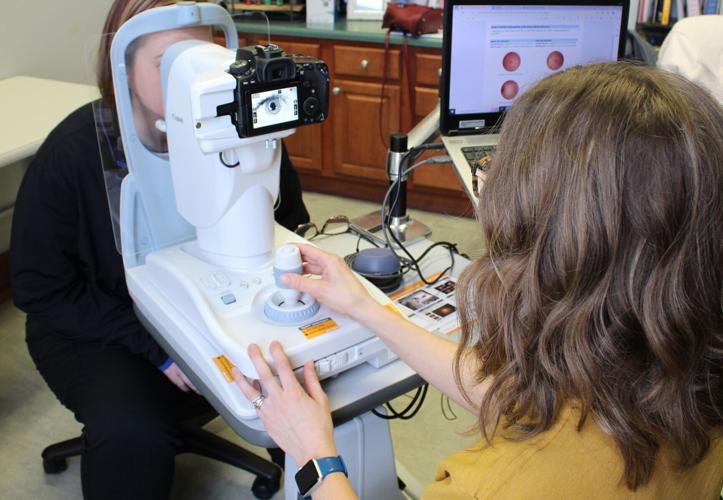
Hastings Family Care in Hastings, Nebraska, part of Mary Lanning Healthcare, recently began using Eyenuk’s EyeArt technology, a special camera connected to a computer backed by machine learning that allows providers to screen patients with diabetes for diabetic retinopathy, without dilating their eyes.

Hastings Family Care in Hastings, Nebraska, a primary care clinic that's part of Mary Lanning Healthcare, is using a new device that uses a type of artificial intelligence to screen patients with diabetes for diabetic retinopathy, without dilating their eyes. It's one example of the kinds of artificial intelligence technologies that are already working behind the scenes in Nebraska hospitals and clinics.
People who have diabetes are advised to have their eyes checked once a year for the condition, which can cause vision loss and blindness. Early treatment can stop progression.
But Jessica Sutton, clinic manager, said a lot of diabetics don’t get the annual exams, often due to a lack of vision insurance, transportation or time to get to an eye doctor. The clinic saw 980 patients with diabetes last year, 45% of whom had not had the exam. Funding for the equipment came through a local donor and a grant UNMC received to improve diabetic care in rural areas.
Dr. Zachary Frey, director of primary care, said he saw three such patients Wednesday morning. One didn’t have insurance. The other two hadn’t had an eye exam in “a while.” Having the device allows the clinic staff to catch such patients when they’re already in the office.
Frey said the system essentially provides three results, each of which triggers next steps. If no problem is detected, the patient is cleared until the next year. If the scan shows changes suggesting retinopathy, the patient is referred to an eye doctor for further investigation. If it detects vision-threatening retinopathy, the patient is sent to a retina specialist.

People who have diabetes are advised to have their eyes checked once a year for diabetic retinopathy, which can cause vision loss and blindness. Early treatment can stop progression. Here, Hastings Family Care is using a new device that uses a type of AI to screen patients with diabetes for the condition, without dilating their eyes.
The systems also can be used to keep patients from falling through the cracks in other ways.
Methodist, for instance, has several systems aimed at helping put additional eyes on lung scans.
One searches radiology reports from scans of, say, the abdomen, that incidentally catch part of the lung for key words like “nodule.” Those get sent to a team that determines whether there might be a problem, and if so, contacts the patient’s doctor, even those in other health systems, said Dr. Adam Wells, a pulmonologist with Methodist Physicians Clinic and Methodist Hospital.
That incidental nodule program flagged more than 13,000 scans last year, which triggered nearly 1,000 communications with a physician and ongoing follow-up with more than 700 patient scans, he said. Those identified nearly 30 cancers.
The health system also screens patients with a known risk for lung cancer using low-dose CT scans, Wells said. While radiologists read the scans, an AI program reads behind and categorizes any spots it sees. Nearly 20 cancers were identified last year out of more than 2,300 scheduled screening scans.
Cancer is a common focus. Locally, the Omaha-based MRI medical device company Bot Image, founded by entrepreneur Randall Jones, last year received FDA clearance for an AI-driven software system called ProstatID for detection and diagnosis of prostate cancer.
But there are others. Leitch said CHI uses robotic process automation, or bots, which use sets of rules to identify patients with upcoming visits and check if they’re due for a test, such as a lung cancer screening.
If so, it places a pending order in the patient’s electronic medical record. If the doctor and patient decide it’s not the right time for the test, the provider can remove it. But it takes the burden off the doctor to remember every test a patient might need, particularly on busy days with lots of distractions.
Other systems can be used to help monitor hospitalized patients. Bryan for several years has used a fall-prevention system developed by Lincoln-based Ocuvera, Ojeda said. It uses 3-D cameras and an algorithm to predict patient movement and alert nurses before a fall can occur.
Epic Systems, she said, has developed five different predictive models that monitor hospitalized patients for other risks, including sepsis and hospital readmission, and alert clinicians so they can respond quickly.
Health systems that use Epic’s health records, including Bryan, CHI and Nebraska Medicine, can then adopt them and build them out for their patient populations, she said.
One of the latest, which CHI has adopted and Bryan is developing, is a model that helps predict when patients will be no-shows for clinic appointments.
If providers can head off missed appointments by, say, Leitch said, providing transportation, they can keep patients healthier.
“If we do what the evidence shows us, as we learn more and more, it’s going to make it easier for us to deliver the care the right way every time,” Leitch said.